This story originally appeared on KERA Breakthroughs.
Nearly half of kids who are born deaf today use cochlear implants. Unlike hearing aids, these surgically implanted devices send signals directly to the nerves you use to hear. And while the electronic components have made it possible for many kids to hear, the surgery doesn’t work for everyone. Which is why some families are so excited about a new hearing technology, the auditory brainstem implant.
For five years, Jiya Bavishi couldn’t hear.
Now, all she wants to do is say hello.
The six-year-old is bouncing around the room in a bright pink top, her tiny gold earrings flash as she waves her arms and uses sign language to talk about the ice cream her father bought for her.
Linda Daniel, a certified auditory-verbal therapist and rehabilitative audiologist with HEAR in Dallas has been working with Jiya since she was a baby. At around twelve months, doctors gave Jiya cochlear implants –but they didn’t work.
“The physician was able to get all of the electrodes into her cochlea,” Daniel says, “however, you have to have a sufficient or healthy auditory nerve to connect the cochlea and the electrodes up to the brainstem.”
Essentially, Jiya’s connection between the cochlea and the brainstem was too thin. There was no way for sounds to make that final leg of the journey and reach her brain.
An Experimental Procedure
Now usually, the story would end here. If cochlear implants don’t work, you turn to sign language. And the Baveshi’s did. But they also heard about an experimental procedure called an auditory brainstem implant.
“This is a very rare procedure,” says Dr. Daniel Lee, “There have been less than 200 of these implanted worldwide in children.”
Lee is director of the pediatric ear, hearing and balance center at Harvard Medical School.
“Surgeons in Europe have pioneered the use of the auditory brainstem implant in children who are born deaf and can’t receive a cochlear implant,” Lee says. “And those data look pretty encouraging.”
In 2013, the FDA approved a clinical trial in the U.S. The surgery skips over the cochlea all together, and goes right into the brainstem. The Baveshi’s needed to decide about brain surgery.
“So at that point the family was at a real crossroads,” Daniel says. “Did they want her to have the option to hear for the rest of her life or did they want the risky decision and have the experimental procedure done?”
The Baveshi’s went ahead with the 8-hour surgery.
A Headband, And A Microchip
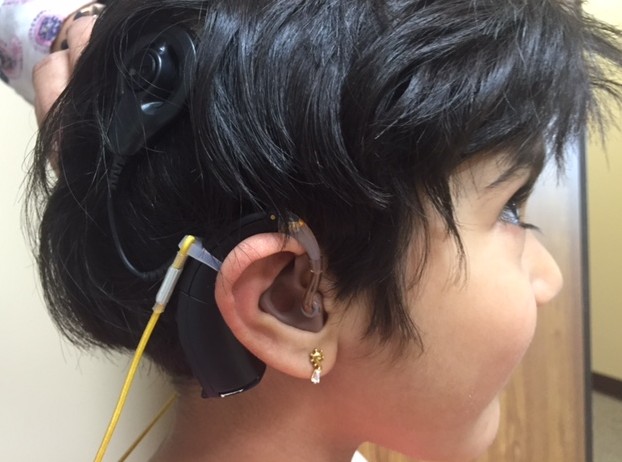
Jiya’s mom, Jigna, pulls back a purple headband to reveal two of the three parts of the device.
There’s the piece that sits on her ear, which works like a microphone to pick up sounds. That microphone is attached to a small black magnet that rests on her head. What you can’t see – the part that magnet transmitter is connected to, is below the skin. A receiver and a tiny microchip in the brainstem.
“It’s a rectangular shaped element,” says rehabilitative audiologist Linda Daniel. “It has two rows of electrodes and each electrode is responsible for a band of frequencies.
From the low frequencies of speech, to the mid, all the way to the high. Still, Daniel says we don’t know exactly what Jiya hears.
“I think we could assume that it doesn’t’ sound crisp, distinct, clearly interpretable,” she says. “It would take longer to learn to interpret the sound.”
Doctors told the Baveshi’s not to expect anything for a year or two. But Jiya didn’t take that long to start recognizing and mimicking sounds.
“They actually had to tell us even though she’s doing so good right now, we have to still be careful where we set our expectations,” says Jigna Baveshi, Jiya’s mom.
Doctors will monitor Jiya, and a handful of other children in the trial, for the next few years. They’ll be studying how her brain develops and incorporates sounds and speech for the first time.