From KUT:
Just after sunrise, young children wearing colorful backpacks start walking into Live Oak Elementary School in Austin. At the door, the principal and the school counselor greet each child by name.
“It’s really important to be able to say their name to help them feel welcome,” counselor Elise Harris said. “You can catch kids who maybe have had a rough morning. There was a student this morning who was in tears, actually, who I tried to engage with.”
Harris invited the child who was upset to come and speak to her in her office. Teachers can also send kids to Harris if they notice an issue.
“Prevention education is really the biggest part of what we do,” she said. “As a school counselor the emphasis is teaching children how to identify and manage their feelings.”
Common concerns are anxiety, depression and behavioral problems. Harris said many students need much more than a school counselor can provide, but families have struggled getting appointments with mental health therapists.
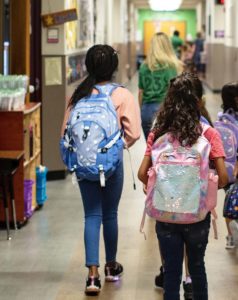
Children walk down a hallway at Live Oak Elementary School in August.
Photo by Gabriel C. Pérez / KUT
“There’s a huge waiting list for therapists, especially for psychiatric services,” Harris said, “and that’s the big problem.”
The Meadows Mental Health Policy Institute reports one out of three Texas children experience a mental health disorder within a year. But because of a shortage of mental health practitioners, many children are unable to get treatment or have to endure long wait times. In Central Texas, experts tell KUT that even with health insurance, children can expect to wait about six months before being seen.
That’s why Harris was thrilled when a state telehealth program called Texas Child Health Access Through Telemedicine, or TCHATT, reached her school in 2021.
“It was just so great to be able to tell parents, ‘Hey, guess what? Your child can see a therapist at school, online at no cost to you,’” she said.
In 2019, Texas lawmakers were presented overwhelming statistics that pointed to a mental health crisis among children coupled with a difficulty in accessing care. As a result, the Texas Child Mental Health Consortium was created. The consortium is made up of medical schools and universities with health programs as well other experts in the mental health field. Together they created, TCHATT and are utilizing 12 higher education health institutions across the state to provide psychiatrists, psychologists, licensed clinical social workers and licensed professional counselors for telehealth appointments. Dell Medical School serves the Austin area.
“We are in 29 different school districts. We have a 13-county catchment area in Central Texas,” said Dr. Nithya Mani, the associate director of the TCHATT programs at Dell Medical School and a pediatric psychiatrist. “I see kids on a daily basis who would never be able to find their way to a child psychiatrist, and that to me is really huge.”
The overall span of the program has grown to encompass more than 3,000 schools across the state reaching both urban and some rural areas.
» MORE: Expanded mental health services on the way for West Texas children
Harris said a typical wait time for a TCHATT appointment is two weeks. However, if the mental health concern is urgent, the child can be seen the same day. Children are matched with the type of therapist appropriate for their needs and typically will have five to six appointments at no charge. If additional care is needed, parents are guided toward resources.
School counselors are trained to coordinate appointments. Their first step is to get approval from parents before making a referral to the health institution. Parents join most appointments, even if just for a short time.
“I’ve had parents who would join while they were working,” Harris said. “They didn’t have to drive anywhere. They just got on their phone or on their computer. So, it’s very doable for parents, and I think they’re very relieved and grateful.”
School counselors typically set up a computer in their office where the child logs in for a private appointment with the therapist. Mani acknowledges the loss of in-person connection, but said the therapists use various tactics to engage.

A laptop is set up in Harris’ office that allows students to connect with mental health practitioners at Dell Children’s Hospital.
Photo by Gabriel C. Pérez / KUT
“I have some clinicians who will do icebreakers and play some kind of game online,” Mani said. “They share screen with a lot of fillable forms so that the student can actually be typing into the form as they’re talking through what coping skills they’re going to use or what’s going to go into their safety plan.”
Mani said the most common reasons for referral are depression and anxiety. But, she clarified, the reason for the referral may be different than the diagnosis, or the outcome of the evaluation.
For example, Dr. Mani said through TCHATT, a therapist found one child who was thought to have ADHD was actually just having trouble with a language barrier. A plan was created to help the situation.
Psychiatrists are also able to prescribe needed medications immediately. Prior to TCHATT, the law required an in-person visit before medications could be prescribed. Coincidentally, this same flexibility occurred after COVID-19 broadened laws on how doctors could engage with patients via telemedicine in Texas.
Harris said students are comfortable using the video conference format, since they spent so much time using it when the COVID-19 pandemic forced schools to teach virtually. Harris said she is grateful for the increased access TCHATT offers.
“If we don’t intervene early, it has larger ramifications down the road,” she said. “Those mental health concerns are going to get bigger. It impacts their education. It impacts their social life. It impacts the family and their family home life. It impacts their social, emotional well-being. It impacts everything.”
Now that TCHATT is in Harris’ school, she said she feels less overwhelmed knowing she can teach students how to manage emotions and refer them to medical mental health care as needed.
“It gives me hope to know that there is this community resource available to us,” she said, “and that the kids don’t have to struggle.”