Thousands of low-income Texans living with HIV are in danger of losing access to medication, as state administrators try to solve a budget deficit crisis worsened by the COVID-19 pandemic.
The state-run Texas HIV Medication Program has asked the legislature for more than $100 million over the next two fiscal years, without which administrators say they’ll be forced to limit eligibility in Texas and reduce HIV prevention efforts. The state already has some of the strictest requirements in the country.
Demand for the program skyrocketed during the pandemic because of job losses in the HIV community. Enrollment has increased by about 30%, now covering more than 21,000 people statewide. The most recent data, from 2018, showed around 94,000 Texans diagnosed with HIV.
“People who are losing their jobs, they may have gone to a private doctor or had insurance,” said Januari Fox, policy director at PRISM Health of North Texas. “They no longer have that and they’re looking for alternatives.”

Josh Mica and his dog Bear at his home on March 21, 2021. Mica, an HIV activist from Acres Homes, said if he can’t afford drugs to manage the virus, he’ll just stop taking them.
One of those stakeholders is Josh Mica, an HIV activist from Acres Homes, who has been relying on this treatment for the last three years. When he was first diagnosed in 2018, tests showed that his viral count was in the millions. He couldn’t stop vomiting because everything he ate tasted like metal.
Doctors now have him on three HIV medications that have dramatically improved his health, he said. He walks up to 10 miles a day as the owner of a dog-walking business.
Mica’s viral load is undetectable, meaning he can’t transmit the virus to another person. But he’s nervous that might change if he gets cut from the program. He doesn’t have insurance, and can not afford to pay for his drugs out of pocket.
“It’s just astronomical,” Mica said. “Like, who can afford $1,500 to $2,000 a month for medication?”
If he can no longer afford the drugs in Texas, Mica said he just won’t take them. Instead, he said he’d deal with severe health consequences of the virus, while fighting for his community.
“People are like ‘oh, just move to another state,'” he said. “I have my whole life here. I have my business. I’m lucky that I just bought a house. I’m not leaving Houston.”
A full year of these drugs costs the program $16,000 per person, according to DSHS — and costs are rising every year.
Mica said there might be other drug assistance options, but it will take time to find a longterm solution.
“If I go six months without my medication, there’s no telling that the medication I was on previously will work,” Mica said. “It decreases my health. I end up in the hospital with no insurance. So my body will just deteriorate because the government is trying to play politics with my life.”
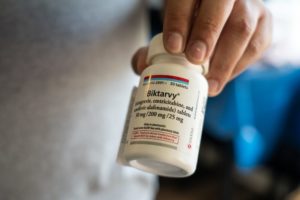
Josh Mica displays his HIV treatment medication, Biktarvy, on March 21, 2021.
This gap in treatment is a concern to physicians and public health workers. Dr. Thomas Giordano, the medical director at Thomas Street Health Center in Houston, said HIV patients need to take their medication continuously. Otherwise, he said, the drugs can become less effective.
“There is no recommendation ever in the U.S. to stop someone’s HIV medicine for a prolonged period,” Giordano said. “There’s no safe time to be off medications.”
Thomas Street, one of the biggest HIV clinics in the state, serves some of the most vulnerable individuals in Harris County. When some patients were cut from the program in December, the safety net clinic had to dip into special funds in order to keep treatments going. Even though coverage has returned, some have likely fallen through the cracks.
“I’m glad they reversed the policy, but it doesn’t reverse the short-term harm,” Giordano said. “People on the fringes, or they’re homeless, they have other problems in their life that are bigger than taking pills necessarily. They want to do it. But if you tell them no, sometimes that no can have a lasting impact.”
The budget deficit is also putting HIV prevention efforts in jeopardy — efforts that have also been greatly impacted by the pandemic. Harris Health System, the county’s safety net system which includes Thomas Street, has seen major dips in HIV testing over the past year.
Dr. Natalie Vanek — chair of the HIV Medication Advisory Committee, which advises DSHS on the treatment program — said in a “resource-rich state” like Texas, lawmakers should be able to find the money to keep these life-saving drugs in the hands of those who need them the most.
“We have rural communities that have very poor access to health care to begin with,” Vanek said. “This is just shameful to talk about.”
Sara Willa Ernst is a corps member with Report For America, a national service program that places journalists into local newsrooms. Sara’s work at Houston Public Media is made possible with support from KERA in Dallas.