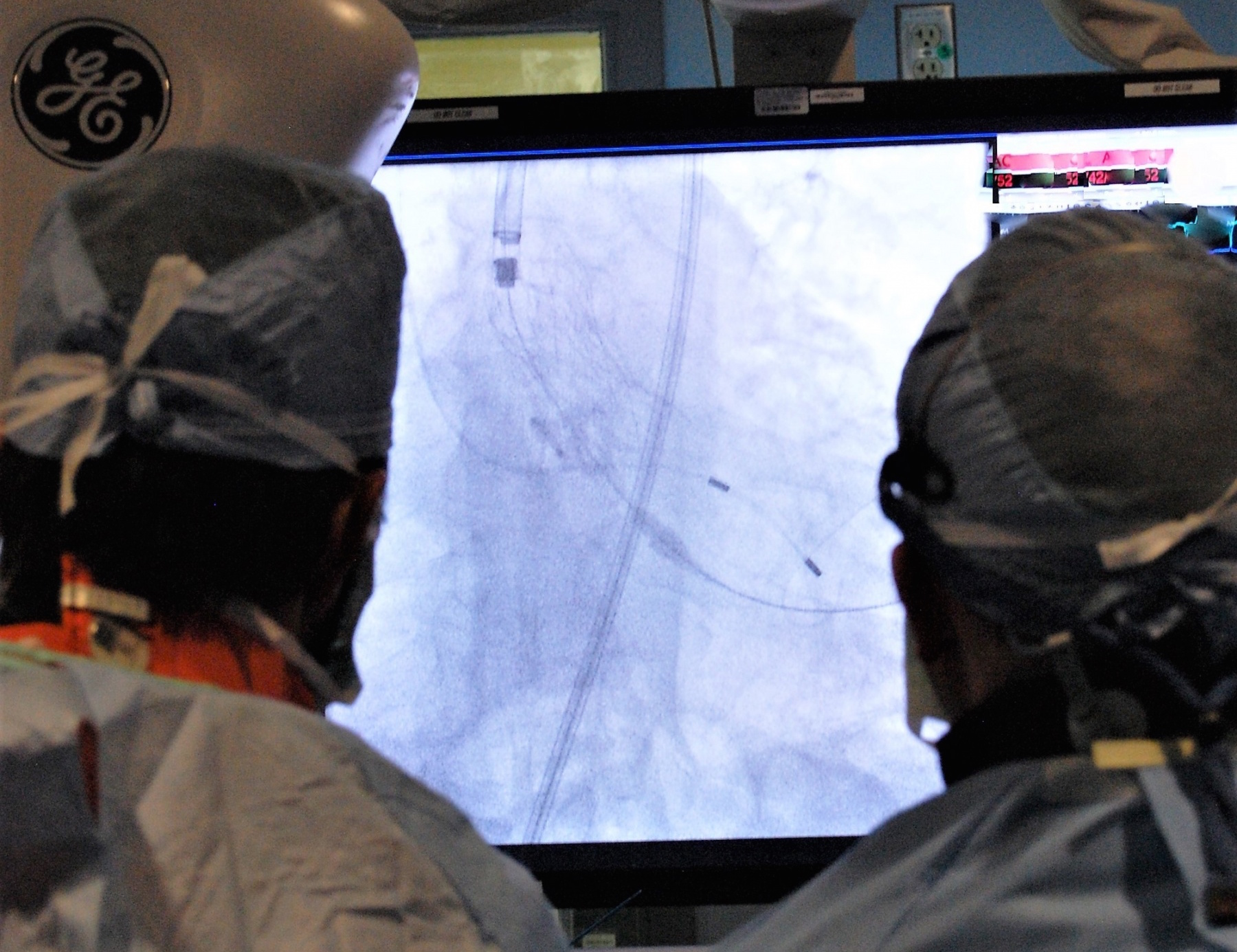
After 15 years of development, the Food and Drug Administration just approved an alternative to open-heart surgery. The new procedure, Transcatheter Aortic Valve Replacement, or TAVR, requires a mere needle stick, which means big changes for patients and surgeons.
Dr. Michael Mack is medical director of cardiovascular surgery for Baylor Scott & White Health, and was a co-principal investigator on one of the procedure’s clinical trials. Mack says the procedure starts with a needle stick in the leg through which the surgeon can thread a valve all the way up to the heart. The old procedure required the surgeon to divide the breastbone, stop the heart and sew in a new valve.
“You can thread this up from an artery in the leg,” Mack says.
Plus, he says the procedure takes much less time – only about 30 minutes – compared to four hours for open-heart surgery. And the recovery time is shorter, too.
“This can be done, most of the time under local anesthesia,” Mack says.
He says this process is similar to how surgeons insert stents in arteries. But it took researchers about two decades to adapt that process to heart-valve replacement.
This quicker, less-invasive procedure is also less expensive. Mack says right now, hospitals will most likely either break even, or possibly even lose money performing it. But he says hospitals are supposed to be committed to serving the patients’ best interests, regardless of financial incentives.
“[Hospitals] have to figure out the financials after the fact,” Mack says.
He says the procedure is innovative but not “exciting.” That’s important; effective medicine should be “nice and boring and routine,” he says. But he still marvels at how much the procedure has evolved since he started his career 35 years ago.
“I’m still in awe of it every time that I do it,” Mack says.
Not everyone who needs heart surgery is eligible for TAVR. Generally, Mack says that means people with certain “anatomy problems” for whom threading the valve through the artery might be difficult. But a majority will be eligible.
“I would say about three out of four patients with this disease, aortic stenosis, will be candidates for this,” Mack says. “For patients, it’s important that they go to a center that offers both options, and they have an experienced team that they meet with.”
This post has been updated to reflect that Mack is medical director of cardiovascular surgery for Baylor Scott & White Health, not Baylor Health Care System.
Support for Texas Standard’s ”Spotlight on Health” project is provided by St. David’s Foundation.
Written by Caroline Covington.