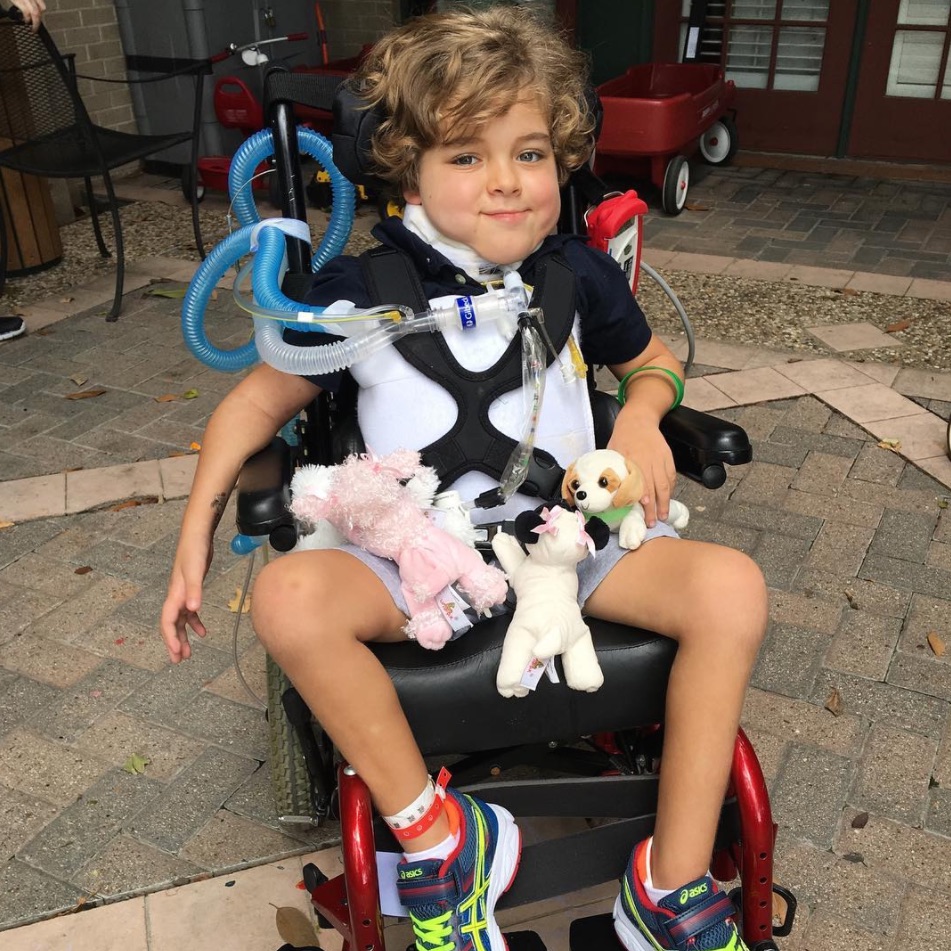
Back in 2016, Rachel Scott noticed her 5-year-old son Braden wasn’t acting like himself over the July Fourth weekend.
“We were celebrating with friends, doing fireworks, going swimming, and he didn’t want to participate in any of those things. He was sleepy, he threw up when he tried to eat and we kind of noticed he was having some trouble swallowing,” Scott says.
As he got weaker over the next few days, Rachel took Braden to an urgent care clinic. When antibiotics and steroids didn’t help, they took him to a Beaumont hospital.
“At that point we had been told he had strep, we had been told he had mono, we figured his throat hurt and that’s why he couldn’t swallow,” Scott says.
But then Braden stopped breathing. He was airlifted to Memorial Hermann Hospital in Houston, and Scott says that’s where doctors finally began looking at neurological causes.
“They had intubated him and put a breathing tube down his throat so that they were doing all the breathing for him,” Scott says. “They tried to take the tube out and let him breathe on his own and he couldn’t take a single breath. So, when they did that, that’s when everything sort of switched for us because there was no good reason that he wouldn’t be able to breathe on his own.”
Doctors said Braden might have a rare disease like Guillain-Barré syndrome or something called anterior horn cell disease. Scott says all of those things sounded scary. But the truth was actually worse.
“Eventually, they told us it was something called acute flaccid myelitis, which, as it turns out, was the worst diagnosis that we were handed in terms of a recovery,” Scott says.
There are no proven treatments for acute flaccid myelitis, or AFM. Over the past five years, there have been hundreds of cases of the disease, which is rare and debilitating. It leads to the sudden paralysis of one or more limbs, and sometimes the paralysis of the muscles used to breathe or swallow. For Braden, this meant that initially, along with being placed on a ventilator and a feeding tube, he could only use the fingers on one hand.
Braden and his mom spent months at a Dallas rehabilitation hospital while has dad cared for Braden’s three siblings back in Beaumont. Eventually, they were able to go back home. But Braden was far from recovered.
“We came back 7 1/2 months later, in February, in an ambulance, and I mean, it was just surreal to think about when I carried him out of the house that day that he’d come back 7 1/2 months later in an ambulance,” Scott says.
AFM is characterized by damage to a certain part of the spinal cord. Although such paralysis is not new and can have various causes, the pattern of outbreaks that have been occurring since 2014 is new. Large spikes in cases have occurred in two-year cycles since then, affecting mostly children. Dr. Benjamin Greenberg says it points to a new virus, or the mutation of an existing one. He studies rare neurologic diseases at the University of Texas Southwestern Medical Center.
“We are now adding to the list of possible causes a virus that, until [the] 2009 to 2014 range, somewhere in there, has not circulated widely, especially within the United States, and when it was circulating was not capable of causing paralysis like it is now,” Greenberg says.
Greenberg is talking about enterovirus-D68, or EV-D68. He says it’s mutated in recent years, and has been shown to cause paralysis in mice in its current form. But Greenberg and other experts agree that more research is needed to understand the virus. Even though many AFM cases occur after a mild respiratory illness – which could be caused by EV-D68 – the virus has only been detected in the spinal fluid of a few AFM victims so far.
Since 2014, the Centers for Disease Control and Prevention, or CDC, says 542 cases of AFM have been confirmed across the country. Cases are generally increasing. Last year, during a so-called spike year, there were 215 confirmed cases – compared to 35 cases in 2017 and 149 in 2016.
Texas tends to have high case counts relative to other populous states, with 29 confirmed cases in 2018. No one knows why this is, but Greenberg says it may be due to better reporting.
“One argument is that our reporting is better than the rest of the country because we have a center dedicated to this, and every time we see a case, we report it and close the loop on that reporting,” Greenberg says.
The CDC was concerned enough about the nationwide increase to create an official incident response team in 2018. Dr. Thomas Clark leads that team.
“There’s still uncertainty, really, as to what AFM is exactly. We’ve defined it for surveillance purposes in order to count cases, but we continue to review that and make sure that’s the right definition and make changes to our case definition if we need to,” Clark says.
The CDC also created a task force of experts who advise the agency and share research. Clark says one of its goals is to better understand the long-term impact on kids.
“There are many kids now living with AFM, some of whom are really seriously affected. We don’t know how many those are, what proportion of kids recover fully, what proportion have ongoing effects, and, especially, what can be done that helps them regain function,” Clark says.