From KERA:
There are a number of differences between the shelters housing Harvey evacuees and the ones where victims of Katrina went 12 years ago. A big one is telemedicine. Children, especially, are being treated by doctors in remote locations.
Nurse Laura Link has helped care for kids at shelters in Baton Rouge after Hurricane Katrina and in Dallas after Hurricane Gustav in 2008. Both times, the challenge was the same: deciding whether to send a sick kid to the emergency room.
“Normally, if a child came in and they’re having an asthma attack, the doctors would say ‘Get them to the Children’s ER.’ Well, what that does to the family is it separates them,”Link says.
“These children have already been displaced,” she says “they’re scared to death and we’re going to pick them up out of a place that’s becoming familiar and plop them into a busy ER?”
One way to avoid that trip to the ER is with a virtual doctor’s visit.
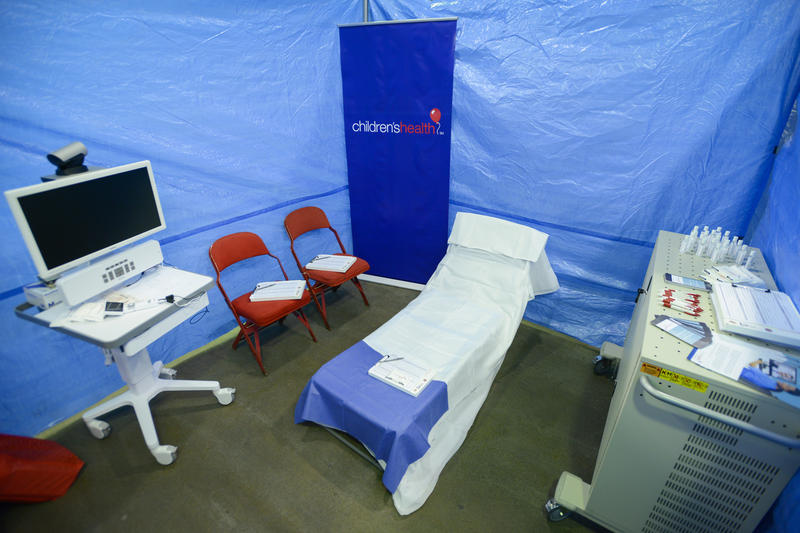
Link, who oversees virtual medicine for Children’s Health in Dallas, spent last Tuesday setting up a virtual visit room at the downtown Dallas mega shelter inside the Kay Bailey Hutchison Convention Center.
Within hours, her team created some privacy with a blue tarp, got an internet connection and hauled in a rolling cart with a big screen and digital medical instruments — all designed to connect kids at the shelter with emergency room physicians at Children’s.
“Our Children’s emergency room specialist can listen to that child through the special stethoscope, he can see them over video, he can talk to them, he can get history from Mom and then, he can collaborate with the doctor,” Link says.
The next challenge was staffing. If a kid gets a bad stomach ache in the middle of the night and needs to see an emergency room doctor, someone still needs to make the appointment, prep the equipment and assist the volunteer doctor at the shelter with using the telemedicine tools.
The shelter’s medical staff is already busy, Link says, so she came up with another idea: a collaboration with the Texas State Guard soldiers.
“I don’t know that this has ever happened,” Link says about the partnership.
The clinic’s State Guard members are medically trained. They’re EMTs or nurses or medics, so all Children’s Health staff had to do was train them on the telemedicine process. Now, when a sick kid shows up, the Guard soldiers take vitals, coordinate the consult and assist the doctors with the remote virtual visit.
“When it’s time for the actual consult, they radio that physician and say ‘We’re ready for you.’ He walks down, steps in front of the camera, goes live, has the consult and then gets right back to taking care of other patients,” Link says.
More time with patients, less on process. Dr. Maeve Sheehan, chief of inpatient services at Children’s Health, says the technology is also helpful for the health care providers at the shelter who have questions about treating children.
“Because children are not small adults, the kinds of medicines used for adults are not appropriate for children,” Sheehan says.
Sheehan says the health impact of a disaster like this on a kid’s health could be different from an adult. And she worries about children who are already sick who might not have access to their medications for weeks.
“Even if we provide acute services in the short term, we need a long-term plan for how are we going to manage this,” she says. “Because [children] will continue to be affected long after the water has receded, both mentally and physically.”
Sheehan expects there will be three kids for every adult who shows up at the shelter. That means there will be plenty of chances for doctors and soldiers to use telemedicine — and keep families together after the storm.